Spondylolisthesis (pronounced spon-di-low-lis-THEE-sis) is a spinal condition where one vertebra sits slightly forwards or backwards relative to the vertebra below it, often because there is more movement at that spinal segment than usual. It most commonly affects the lower back (lumbar spine), often at L5-S1 or L4-5. Importantly, many people have spondylolisthesis on imaging and have no symptoms at all. When symptoms do occur, they are usually linked to how sensitive the joints, discs, muscles, and nearby nerves are, rather than the spine being “out of place”.
There are different types. Isthmic spondylolisthesis is often related to a small stress injury or abnormality in a part of the vertebra called the pars interarticularis (many people hear this described as spondylolysis). This can develop in adolescents and young adults, particularly those who do repeated back extension and rotation (for example gymnastics, cricket fast bowling, dance, football codes, and weightlifting). Degenerative spondylolisthesis is more common later in life and reflects gradual age-related changes in discs and facet joints, sometimes occurring alongside spinal stenosis (narrowing around the nerves).
Physiotherapy for spondylolisthesis focuses on helping the area feel stable and resilient again. A physiotherapist can guide you through targeted strengthening and movement retraining, help reduce nerve irritation if present, and build a clear plan for returning to work, daily activities, gym, and sport.
Key Facts
- Across studies, the prevalence of spondylolisthesis in the general population has been reported to be between 6% and 10% (estimates vary by type of slip and imaging method). 🔗
- In adult populations, reported prevalence of asymptomatic isthmic spondylolisthesis ranges from 3.7% to 11.5%. 🔗
- The natural history is generally favourable and only around 10% to 15% of people seeking treatment ultimately have surgery. 🔗
- Reported progression rates in the literature include 34% for degenerative spondylolisthesis, 32% for congenital isthmic spondylolisthesis, and 4% for post-traumatic isthmic spondylolisthesis. 🔗
- In athletes with symptomatic pars injuries (a common pathway to isthmic spondylolisthesis), a systematic review reported return to sport at any level of 92% with conservative care, with average time to return of 4.6 months. 🔗
Risk Factors
- Sports involving repeated extension/rotation (gymnastics, dance, cricket fast bowling, some football codes, weightlifting)
- Rapid growth phases in adolescents (load tolerance changes quickly)
- Family history of pars defects or spinal shape differences
- Age-related disc and facet joint degeneration (degenerative spondylolisthesis)
- Reduced hip mobility or poor lumbopelvic control (increases strain through the low back)
- Higher body weight or low overall conditioning (can increase spinal load and sensitivity)
- Jobs or lifestyles with repetitive lifting, twisting, or prolonged standing
Symptoms
- Localised low back pain, often worse with certain positions or loads
- Pain that refers into the buttock or thigh (may feel like “sciatica”)
- Pins and needles, numbness, or weakness in the leg (nerve involvement)
- Tight hamstrings or a feeling of “pulling” behind the thighs
- Pain with back extension (arching) or with rotation, especially in isthmic cases
- Heaviness, cramping, or leg symptoms with walking/standing that eases with sitting or bending (more common with stenosis and degenerative slips)
- A “step-off” feeling in the low back (sometimes noticed on examination)
- In severe cases: changes in walking pattern, reduced balance, or reduced foot strength
Aggravating Factors
- Repeated or sustained back extension (arching), especially under load
- Prolonged standing, particularly with an arched posture
- Walking downhill or long distances if stenosis is present
- Heavy lifting, especially with poor hip hinge control or sudden twisting
- Running, jumping, and high-impact sport during painful phases
- Deep backbends, overhead lifting with lumbar extension, or aggressive stretching into extension
- Prolonged sitting or long car trips (some people, particularly with disc and nerve sensitivity)
Causes
Spondylolisthesis happens when forces across a spinal segment exceed what the local structures can tolerate.
In isthmic spondylolisthesis, the key issue is usually a stress-related change in the pars interarticularis. This can develop from repeated stress (like a stress fracture) during growth or high training loads. Once the pars is weakened on both sides, the vertebra can gradually shift relative to the one below.
In degenerative spondylolisthesis, gradual wear and tear changes in the disc and facet joints can reduce stability. The joints and ligaments may become less effective at controlling small movements, and the vertebra can slowly translate. Degenerative slips often occur with arthritic change and sometimes spinal canal narrowing that irritates nerves.
Less common causes include congenital differences in bone shape (dysplastic), trauma, prior spine surgery (iatrogenic), or bone weakening conditions.
A key point for most people is that pain is not purely about “bones slipping”. Pain often comes from irritated joints, sensitive discs, protective muscle tension, reduced trunk control, nerve irritation, and fear or guarding with movement. That is why physiotherapy for spondylolisthesis can be highly effective even when the slip itself cannot be “put back”.
How Is It Diagnosed?
A physiotherapist can often make a strong clinical diagnosis from your history and a thorough physical exam. This includes identifying patterns such as extension-related pain, load intolerance, painful movement segments, hip stiffness, hamstring tension, and any signs of nerve involvement (strength, reflexes, sensation, nerve tension tests).
Your physio will also screen for “red flags” such as significant weakness, changes to bladder or bowel control, unexplained weight loss, fever, night sweats, or severe unrelenting night pain, which require urgent medical assessment.
Imaging is not always necessary early on, especially if symptoms are mild and improving. However, imaging may be helpful when symptoms persist, leg symptoms are significant, there is concern about a pars injury in a young athlete, or treatment planning depends on understanding the grade and stability of the slip.
Investigations & Imaging
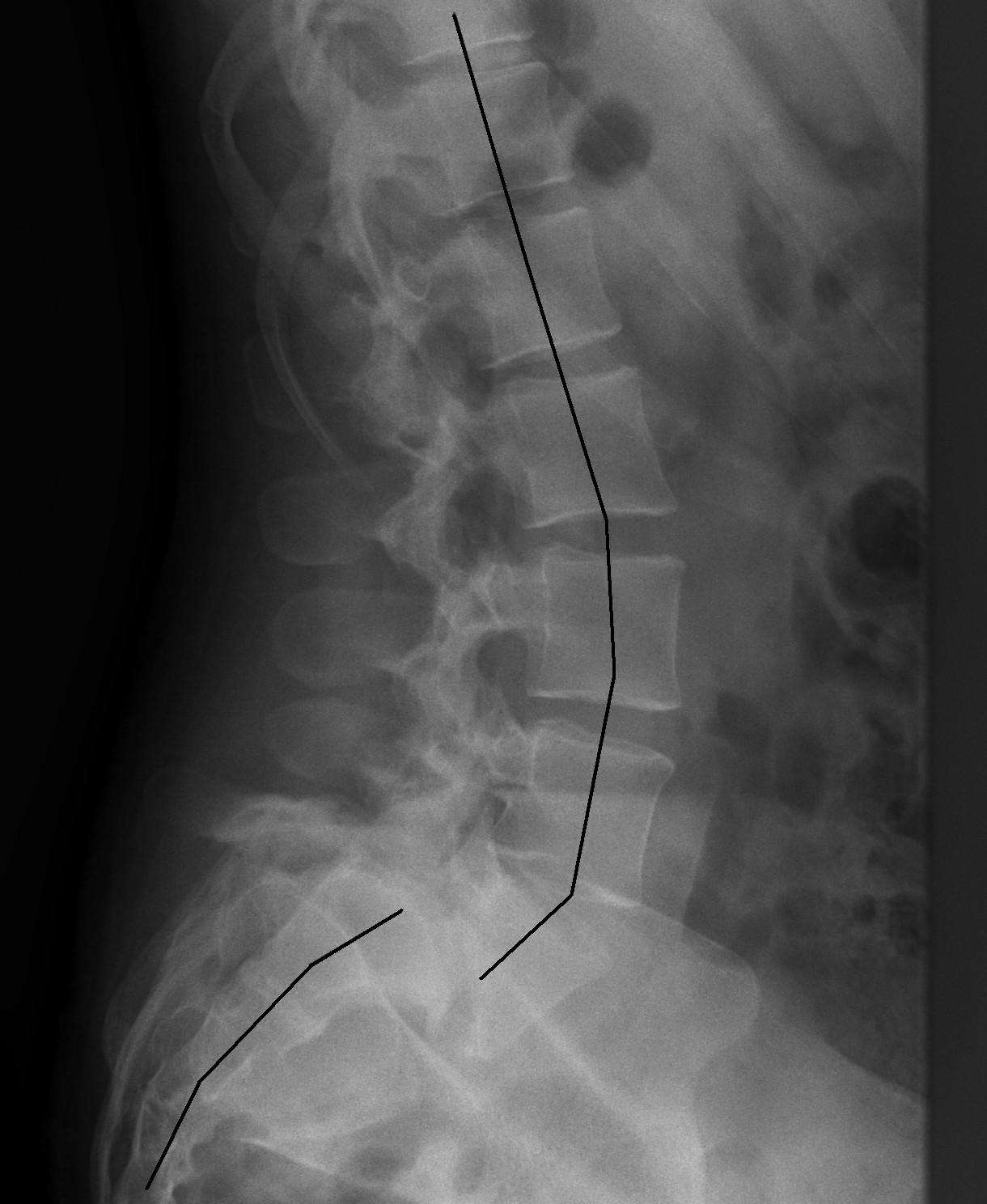
- Standing lumbar spine X-ray (lateral view)
- Shows the presence and degree of vertebral slip, helps estimate the grade.
- Flexion and extension X-rays
- Helps assess whether the segment appears to move more than expected (instability), which can influence management decisions.
- Oblique X-ray or “spot” view (often at L5-S1)
- Can help identify pars defects linked to isthmic spondylolisthesis (not always visible).
- MRI scan
- Assesses discs, nerves, spinal canal narrowing (stenosis), and inflammation or stress changes, and helps when leg symptoms are present.
- CT scan
- Provides detailed bony information, useful for confirming pars defects or assessing bone anatomy when surgery is being considered.
- Bone scan or SPECT (sometimes combined with CT)
- Can help determine if a pars injury is “active” (bone stress reaction) versus old and healed, especially in younger athletes.
Grading / Classification
- Meyerding Grade I
- 0% to 25% slip. Often managed well with spondylolisthesis physiotherapy exercises and load modification.
- Meyerding Grade II
- 25% to 50% slip. Management depends on symptoms, stability, and nerve involvement.
- Meyerding Grade III
- 50% to 75% slip. Higher likelihood of ongoing symptoms; needs careful physiotherapy-led rehab and sometimes specialist input.
- Meyerding Grade IV
- 75% to 100% slip. More complex, with greater risk of nerve involvement and postural changes.
- Meyerding Grade V (spondyloptosis)
- Greater than 100% slip. Rare, typically specialist-managed.
Physiotherapy Management
Exercise
Physiotherapy for spondylolisthesis usually centres on building a strong, well-controlled “support system” around the spine. Early on, your physiotherapist will help you find positions and movements that calm symptoms, then progressively reload the area so it becomes less reactive. This often starts with breathing and trunk control work that targets deeper stabilisers (such as the transversus abdominis and multifidus) without bracing rigidly. From there, spondylolisthesis physiotherapy exercises typically progress into functional strength: hip and gluteal strength (to reduce overload through the lumbar spine), trunk endurance, and coordinated movement patterns for squatting, hinging, and stepping. If leg symptoms are present, rehab may include nerve mobility work, walking programs, and graded exposure to standing tolerance. For athletes and active people, spondylolisthesis rehab includes a staged return to running, jumping, and sport-specific skills, with careful attention to lumbar extension volume, fatigue, and technique.
Activity Modification
Good spondylolisthesis rehab rarely means “stop everything”. Instead, your physiotherapist helps you identify which activities are currently sensitising the area and how to adjust them while you keep moving. In isthmic cases, this often means temporarily reducing repetitive extension and rotation, changing gym choices (for example, swapping heavy overhead work or deep backbends for alternatives), and modifying training volume. In degenerative spondylolisthesis with stenosis features, many people tolerate gentle flexion-based positions and cycling better than long standing or downhill walking early on. The goal is to find a sustainable baseline you can build from, rather than pushing through flare-ups that set you back.
Manual Therapy
Manual therapy is not used to “push the vertebra back in”. Instead, physiotherapists use hands-on techniques to improve comfort and movement options around the affected area. This might include gentle mobilisation of stiff adjacent spinal segments, rib or thoracic mobility work, and hip joint techniques when hip stiffness is increasing strain on the low back. Soft tissue techniques may help reduce protective muscle tension in the back, glutes, or hip flexors, making it easier to retrain movement patterns and progress strengthening. Manual therapy tends to work best when it supports your exercise plan, rather than replacing it.
Postural Retraining
Posture is not a moral issue, and there is no single “perfect posture”. However, some people with spondylolisthesis do better when they learn to reduce excessive lumbar extension during standing, walking, overhead work, or lifting. Your physiotherapist may coach a more efficient ribcage and pelvis position, improve hip hinge mechanics, and build endurance so you can maintain good control when tired. The aim is to reduce repeated pinching and shear forces through the sensitive segment and help you feel more stable in daily life.
Bracing & Taping
A brace is not required for everyone. In some cases, short-term bracing can help settle symptoms, especially if pain is high or if an adolescent has an irritable pars injury alongside early slip. A physiotherapist will guide when bracing is appropriate, how to avoid over-reliance, and how to wean it as strength and control improve. Taping is sometimes used as a short-term proprioceptive cue to help you notice and limit painful extension or to increase confidence during activity, but it should sit alongside a progressive exercise plan.
Heat & Ice
Heat or ice can help manage pain and muscle spasm during flare-ups. Heat often suits stiffness and guarded muscles; ice may feel better for more “hot” or irritated pain. These are symptom tools, not structural fixes, and your physiotherapist will usually pair them with active strategies like walking, gentle mobility, and a graded strengthening plan.
Education
Education is a major part of physiotherapy for spondylolisthesis. This includes explaining what the scan findings do and do not mean, why pain can persist even without “worsening slip”, and how to pace activity so you keep making progress. Your physio will also teach warning signs that need medical review, how to modify lifting and sport technique, and how to respond to flare-ups without losing all momentum. Clear education reduces fear, improves confidence, and usually improves outcomes.
Other
Depending on your presentation, your physiotherapist may also address sleep, stress, general fitness, work ergonomics, and load management across the week. If pain is not settling, your physio may liaise with your general practitioner for medication options, or discuss whether a specialist opinion is appropriate, especially if there are progressive neurological symptoms.
Other Treatments
Other treatments may be used alongside physiotherapy for spondylolisthesis depending on symptoms and irritability. This can include short-term pain relief medication prescribed by a doctor, activity pacing strategies, and in selected cases, image-guided injections to help manage nerve pain or facet joint irritation. For persistent pain, a multidisciplinary approach can help, combining physiotherapy rehab, medical management, and sometimes psychological strategies that target pain-related fear and hypervigilance. These options work best when they support, rather than replace, an active spondylolisthesis rehab program.
Surgery
Surgery is not the first-line option for most people with spondylolisthesis. It is more commonly considered when there is persistent disabling pain despite well-performed conservative care, progressive neurological signs (worsening weakness, reflex changes), significant nerve compression, or higher-grade slips with functional decline. Surgical approaches vary and may include decompression (creating space for irritated nerves) and fusion (stabilising the segment). The specific plan depends on the type of spondylolisthesis, slip severity, instability, and symptoms.
Physiotherapy still plays an important role if surgery is planned. Prehabilitation can improve strength, walking tolerance, and recovery confidence. After surgery, physiotherapists guide graded return to function, rebuild trunk and hip strength, and help you return safely to work and sport, while respecting tissue healing and your surgeon’s restrictions.
Prognosis & Return to Activity
Many people improve significantly with physiotherapy for spondylolisthesis, especially when rehab targets strength, movement control, and graded exposure back to meaningful activity. Symptoms often fluctuate, so the aim is to reduce both pain intensity and flare-up frequency, while building long-term capacity.
Return to activity is based on function rather than a single scan result. A physiotherapist will typically progress you through stages: settling pain, restoring daily movement tolerance, rebuilding strength and endurance, then reintroducing higher loads and sport-specific tasks. If leg symptoms are present, your return plan also considers nerve sensitivity and walking tolerance. With higher-grade slips, rehab often focuses on robust trunk and hip strength, careful extension management, and close monitoring of neurological symptoms.
Complications
- Ongoing nerve irritation causing persistent sciatica-like symptoms
- Spinal stenosis symptoms (leg heaviness, reduced walking tolerance), especially in degenerative cases
- Progressive weakness, altered reflexes, or foot drop (needs urgent medical review)
- Significant flare-ups leading to activity avoidance and deconditioning
- Rarely, cauda equina syndrome (bowel/bladder changes, saddle numbness) requiring emergency care
Preventing Recurrence
- Keep a maintenance program of spondylolisthesis physiotherapy exercises that targets trunk endurance and glute strength, especially if you have recurrent flare-ups or a physically demanding job.
- Limit repeated end-range lumbar extension under fatigue (for example, high-rep backbends, excessive arching during overhead lifts), and build technique that shares load through hips and upper back.
- Progress sport and gym loads gradually after breaks, using planned increases in volume and intensity rather than sudden spikes, which are a common trigger for pars-related symptoms.
- Maintain hip mobility and hip hinge capacity so lifting, running, and change of direction tasks load the hips rather than repeatedly shearing the low back.
- If you have stenosis-type symptoms, manage walking dose intelligently (shorter, more frequent walks, avoid long downhill early on) and build tolerance over time with physio guidance.
When to See a Physio
- Low back pain that persists beyond 1 to 2 weeks, or keeps returning with sport, work, or gym
- Pain that worsens with extension/arching, especially in adolescents or athletes (possible pars involvement)
- Buttock or leg symptoms (pins and needles, numbness, weakness, pain below the knee)
- Reduced walking tolerance, leg heaviness, or symptoms that ease with sitting or bending
- You have been told you have spondylolisthesis on imaging and want a clear plan for safe strengthening and return to activity
- Post-operative rehab planning or guidance after specialist review
