The Anterior Cruciate Ligament (ACL) is an important structure for knee stability, especially in the sporting and active population. This ligament plays an integral role stabilising anterior (forwards) movement of the tibia, as well as excessive rotational movement. Injury to this ligament often occurs with a non-contact change of direction mechanism, however can also occur from direct contact. Like all injuries, there is a grading system to classify the extent of the injury, which will dictate management. Most ACL injuries involve significant damage to the ligament and will require specialist opinion to discuss management options. These options have generally been between operative or non-operative management. A range of factors will determine appropriate management of the injury. These include associated injuries within the knee, age, return to sport/activity goals, comorbidities, costs and personal preference. This will be an important conversation to have with the specialist.
Traditionally, an ACL rupture was considered to have a poor likelihood of healing, therefore warranting surgical intervention to restore structural integrity. However, studies have identified the ACL has a rich blood supply and capacity to heal in certain instances. This has prompted exploration into possible mechanisms in restoring the ligament through non-operative management.
A recent hypothesis regarding non-surgical management of ACL ruptures is the Cross Bracing Protocol. This protocol aims to facilitate the healing of specific ACL ruptures by approximating and reducing the ligamentous tissue whilst using a ROM knee brace.
Reducing the gap distance is achieved by locking the knee in a 90-degree angle for 4 weeks. This is followed by a gradual return to full knee extension in the brace over the next 8 weeks.
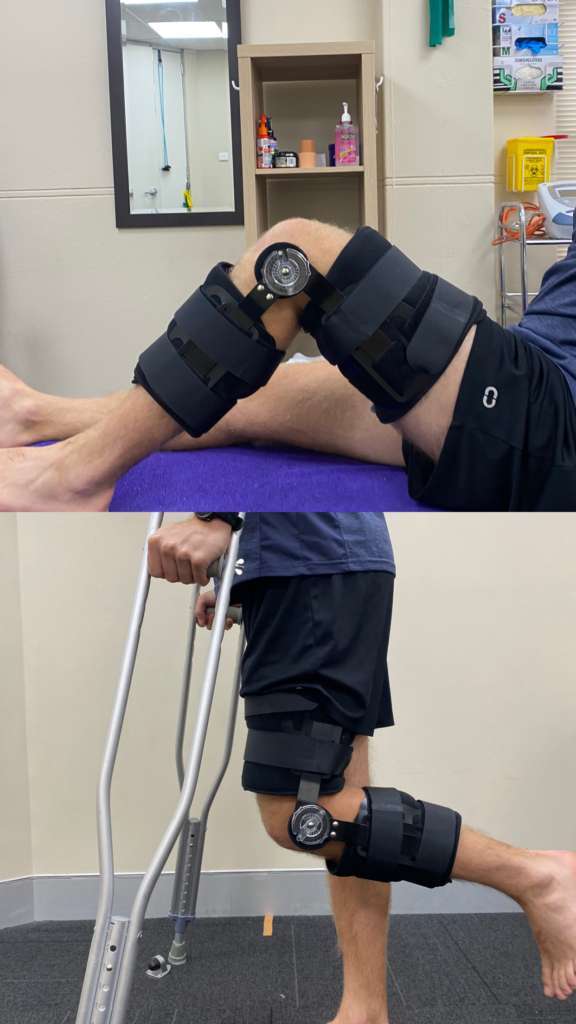
This 12-week bracing period is in conjunction with pharmacological intervention and rehabilitation. Following this period, after imaging and specialist consideration, patients will continue ACL rehabilitation protocol with the aim to return to sport at 9-12 months. Although in the preliminary stages, evidence for this intervention is promising. Further research to build the body of evidence is required, however for specific patients, it’s now an avenue that can be explored.
Suitability
There are a range of factors in determining an individual’s suitability for the bracing protocol.
Histology
Grade 3 tear of the ACL must be present and remain within the synovial envelope, this will be determined by MRI and reviewed by expert radiologist and specialist.
Time since Injury
Timing is a very important factor. The bracing protocol must be set up within 20 days of the acute injury.
History of Clotting Disorders
Bracing for long periods slows blood flow through the veins and therefore increases the risk of a clot forming. For this reason, patients with a history of DVT or strong family history of clotting disorders are not appropriate for this intervention.
Associated Injuries
An acute knee injury can often impact multiple structures within the knee, and this will dictate management. For example, bucket-handle meniscal tears or chondral defects can be associated with ACL ruptures and these patients are not appropriate for bracing due to the specific management required for these complex injuries.
Comorbidities
Clients with other medical conditions or injuries that may impact the compliance and safety of the cross bracing protocol will not be indicated for this intervention. This will be assessed by the specialist and medical team.
In addition to this criteria for suitability, the individuals preference and specific goals must also be considered.
Key Advantages
Promising research supporting the ability of the ACL to heal in certain cases has significant advantages of the management of ACL ruptures. Although low, there are risks associated with surgery for ACLs. The protocol provides a non-operative management option for individuals who have the goal of a possible return to sport. Furthermore, the cost of surgical intervention is a factor in the management process. The bracing protocol may be a viable option for those individuals who would like to return to sport however the cost of surgical intervention has previously been a deterrent. While the evidence is still emerging, this intervention has the potential to be a great option for individuals who meet the inclusion criteria and would prefer non-operative management.
Final Word
Cross Bracing is an exciting new treatment avenue for ACL injuries. There is the potential for another prong to the management of ACL ruptures in specific populations. As previously mentioned there is the need for further research and expert guidelines to ensure the protocol can be implemented safely and smoothly. It must also be reinforced that this protocol is only indicated for specific patients with a specific ACL rupture. For this reason, expert consideration from an orthopaedic specialist, GP, radiologist and physiotherapist are all required in a timely manner to determine the potential for the Cross Bracing Protocol.
References:
Filbay, S.R. et al. (2023) ‘Healing of acute anterior cruciate ligament rupture on MRI and outcomes following non-surgical management with the Cross Bracing Protocol’, British Journal of Sports Medicine [Preprint]. doi:10.1136/bjsports-2023-106931.
